A Proposal to Reduce Malaria Across the Korean Peninsula: Another Opportunity for Inter-Korean Cooperation
Introduction
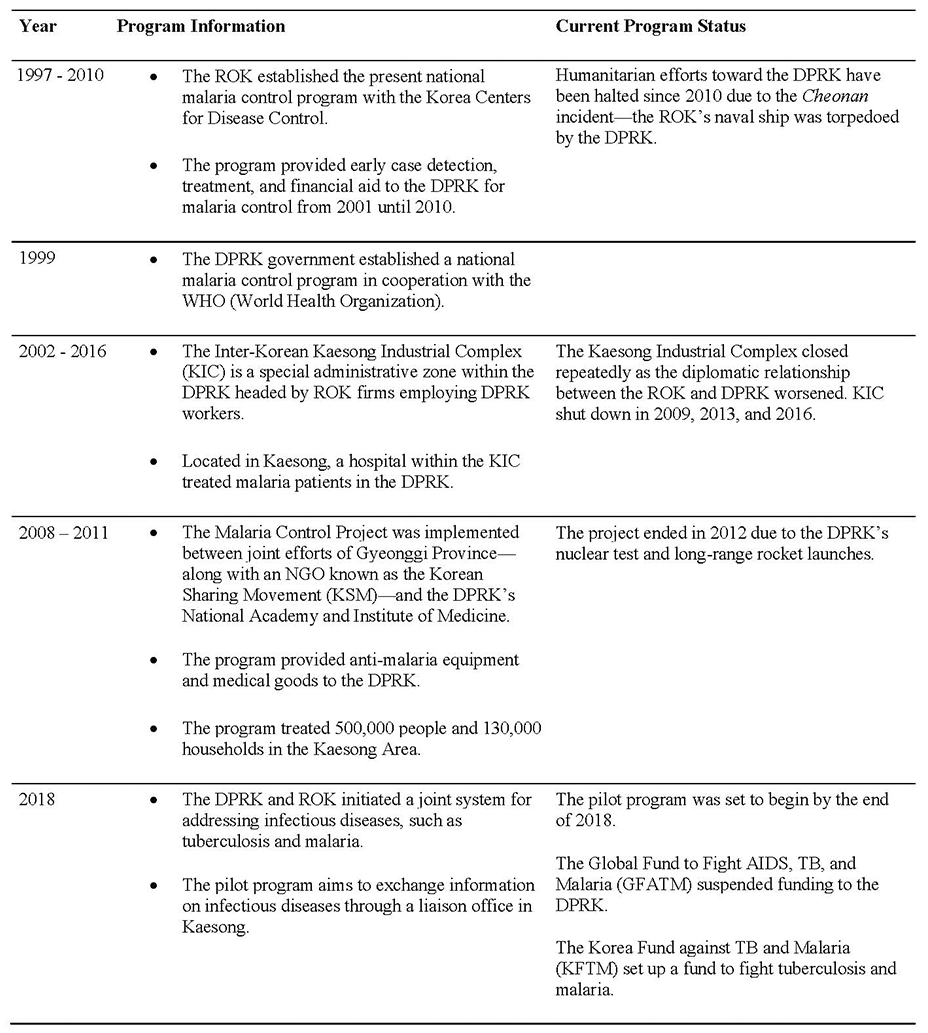
There is a malaria epidemic across the Korean Peninsula, and South Korea (Republic of Korea, ROK) and North Korea (Democratic People’s Republic of Korea, DPRK) have agreed to cooperate to fight this scourge. In September 2018, South Korean President Moon Jae-in and North Korean leader Kim Jong Un signed an agreement on public health collaboration. Two months later the two countries unveiled a plan for a joint initiative to exchange health information through a liaison office in Kaesong near the Demilitarized Zone (DMZ). Both countries hope these exchanges will facilitate more effective responses to malaria incidents. Although this is not the first time that both countries have attempted to jointly tackle malaria, the agreement was a significant leap forward in addressing this public health issue, given that funds and collaborative efforts have been suspended in the past (Figure 2, Table 1).[1], [2], [3]
What’s Behind the Outbreak?
Although malaria cases in the DPRK declined between 2012 to 2015, reports indicate that they surged from 773 in 2015 to 2,184 in 2017, a 182 percent increase within only two years (Figure 1).[4] Likewise, the ROK experienced a resurgence of malaria cases from 2013 to 2016—an overall 56 percent increase from 386 cases in 2013 to 602 cases in 2016 (declining thereafter to 436 cases in 2017).
In the ROK, high numbers of malaria cases most commonly occur along the inter-Korean border at the DMZ, where ROK (and DPRK) soldiers are heavily exposed to low-lying, humid and swampy areas.[5], [6], [7] Some experts have suggested that the rise of malaria cases in the ROK can mainly be attributed to “insufficient antimalarial efforts by North Korea.” It is tempting to assume that infected mosquitos usually fly across the DMZ and infect ROK soldiers, thereby contributing to ROK’s surge of malaria cases. However, there are several epidemiological factors that prevent the identification of a specific cause. For example, many meteorological studies suggest a low probability for mosquitoes flying from the DPRK to the ROK, as the wind blows mainly from south to north in the summer along the DMZ.[8]
A 2016 meteorological study suggests that wind velocity alone is not sufficient to predict the prevalence of malaria.[9] In fact, a multitude of meteorological changes—such as temperature, wind velocity, and humidity—are strong predictive factors of malaria cases in certain regions along the DMZ. Furthermore, the rise in malaria cases in South Korea may be due to antibiotic resistance or genetic diversification of the parasite, which may be due to accumulated mutations and natural selection.[10] For instance, one study demonstrated that 70 percent of mosquitos analyzed from high-risk areas along the DMZ were resistant to insecticides.[11]
Why Cross-Border Cooperation is Critical
Because the spread of infectious diseases is largely influenced by geographic proximity, political cooperation between North and South Korea will be indispensable to addressing malaria across the Korean Peninsula. Although there is an abundance of malaria research studies available in the ROK, there are currently no research articles on malaria from the DPRK.[12] Additionally, the ROK currently uses rapid and highly sensitive diagnostic tests to detect malaria.[13], [14] In contrast, the DPRK has a shortage of diagnostic supplies and a formal prevention program that can accurately assess malaria cases.[15]
The November 2018 agreement foreshadows potential public health solutions, but a malaria prevention program is only as effective as the data that are collected and reported. Thus, it is crucial for North and South Korea to cooperate in establishing standardized indicators or methods for malaria surveillance, particularly along the DMZ, perhaps as part of the liaison office at Kaesong. The source of infections may be difficult to identify, but facilitating cross-border partnerships will be highly beneficial in synthesizing existing data from all surveillance systems regionally in real-time and analyzing data to produce rapid response strategies. This would allow both countries to implement an effective malaria surveillance system that provides customized output solutions to health care stakeholders at local, national, and international levels that help facilitate evidence-based health policies.[16]
Surveillance, Surveillance, Surveillance
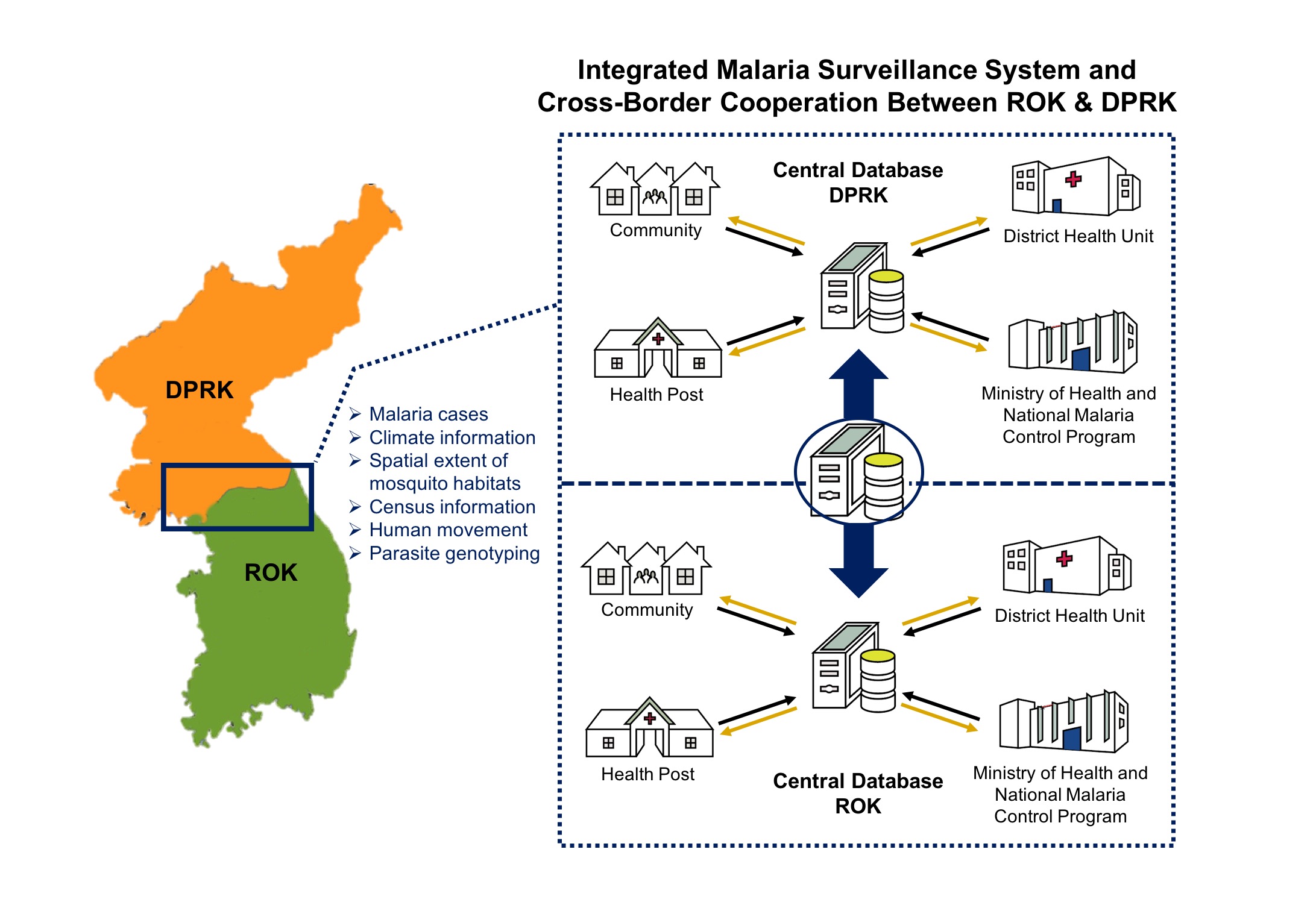
Surveillance is the key to malaria control and eradication, and more information is needed on the origin of malaria cases in Korea before an evidence-based public health strategy can be executed. A strong malaria control program would also feature cross-border data sharing derived from improved surveillance. The model below proposes a surveillance system that could be used in the cross-border region (Figure 3). This model would not only provide real-time information on malaria cases at all health care administrative levels, thereby fostering cooperation and overcoming the limitations of traditional reporting structures; it would also create a shared central database including information on malaria cases, climate, spatial extent of mosquito larval habitats, census information, human movement, social networks, and parasite genotyping. One strategy to address the controversial issue of sharing information on human movement and social networks would be to limit such information to specific malaria cases.
In the final analysis, the two countries are fighting the same deadly infectious disease. It is imperative, therefore, that they overcome political challenges to ensure the greatest amount of cooperation in addressing epidemiological, ecological, and geographical factors that all contribute to the malaria epidemic across the Korean Peninsula.
Table 1. A timeline of the status of cooperation between ROK and DPRK on joint antimalarial efforts.
Figure 1. Estimated malaria cases in the ROK and DPRK.[17]
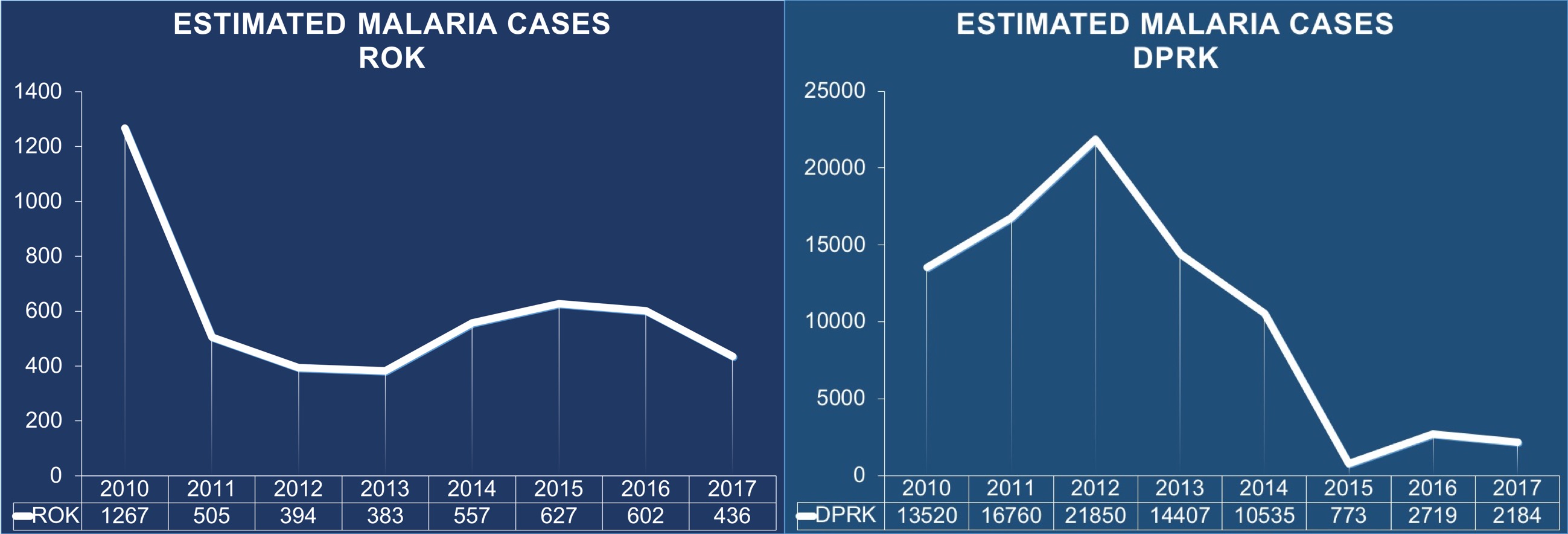
Figure 2. Funding for malaria control in the DPRK by Global Fund.[18]
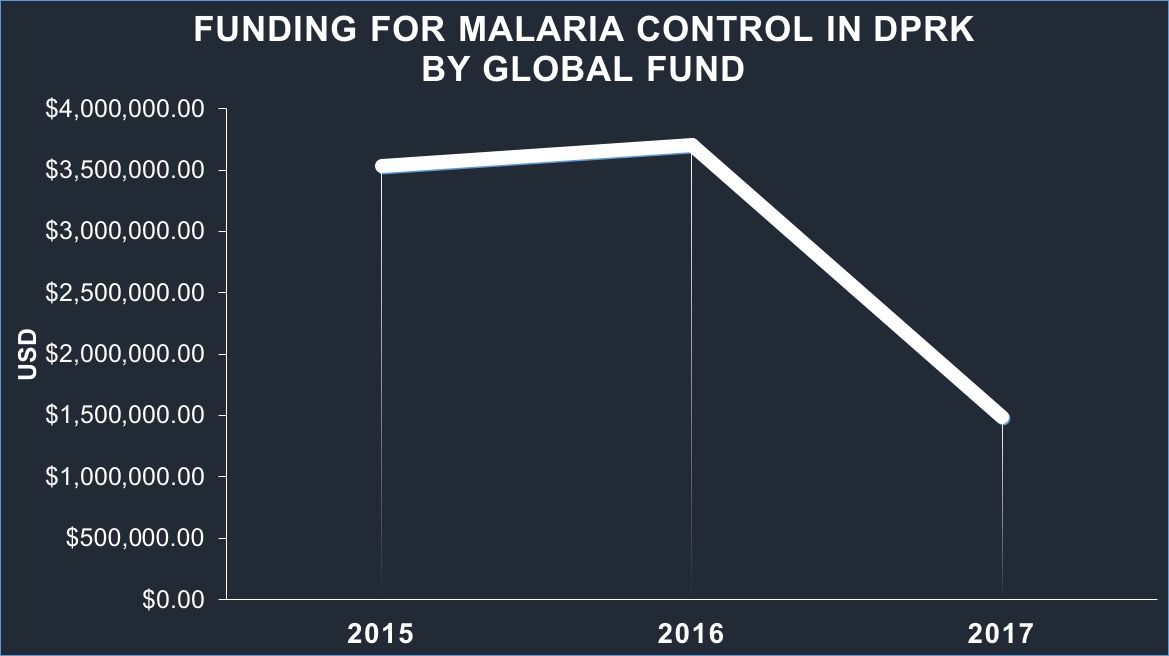
Figure 3. Cross-border malaria surveillance model across the Korean Peninsula.
Acknowledgments
We would like to thank Richard Sokolsky, Elizabeth Park and Jin Qiu for providing their support, comments and suggestions throughout the course of this article.
- [1]
World Health Organization, World Malaria Report 2018, November 2018, accessed April 29, 2019, https://www.who.int/malaria/publications/world-malaria-report-2018/report/en/.
- [2]
Macdonald, Hamish. “North Korea Calls on Global Fund to Reconsider Termination of Grants,” NK News, March 13, 2018, accessed April 29, 2019, https://www.nknews.org/2018/03/north-korea-calls-on-global-fund-to-reconsider-termination-of-grants/.
- [3]
Jung, Da-Min. “North Korea Establishes Global Fund to Fight TB, Malaria,” The Korea Times, September 21, 2018, accessed April 29, 2019, https://www.koreatimes.co.kr/www/nation/2018/09/103_255967.html.
- [4]
World Health Organization, World Malaria Report 2018, November 2018, 134-36, accessed April 29, 2019, https://www.who.int/malaria/publications/world-malaria-report-2018/report/en/.
- [5]
Kim, Heung-Chul, Laura A. Pacha, Won-Ja Lee, Jong-Koo Lee, Joel C. Gaydos, William J. Sames, Hee-Choon S. Lee et al, “Malaria in the Republic of Korea, 1993–2007. Variables related to re-emergence and persistence of Plasmodium vivax among Korean populations and US forces in Korea,” Military Medicine 174, no. 7 (2009): 762-769.
- [6]
Shim, Jae Chul, Dong‐Kyu Lee, Terry A. Klein, Heung‐Chul Kim, Won‐Ja Lee, and Heung Ku Im, “Surveillance of vivax malaria vectors and civilian patients for malaria high‐risk areas in northern Gyeonggi and Gangwon Provinces near the demilitarized zone, Republic of Korea, 2003–2006.” Entomological Research 40, no. 4 (2010): 202-210.
- [7]
Yoo, Dae-Hyun, E-Hyun Shin, Mi-Yeoun Park, Heung Chul Kim, Dong-Kyu Lee, Hyun-Ho Lee, Hyun Kyung Kim, and Kyu-Sik Chang, “Mosquito species composition and Plasmodium vivax infection rates for Korean army bases near the demilitarized zone in the Republic of Korea, 2011,” The American Journal of Tropical Medicine and Hygiene 88, no. 1 (2013): 24-28.
- [8]
Huldén, Lena, and Larry Huldén, “Dynamics of positional warfare malaria: Finland and Korea compared,” Malaria Journal 7, no. 1 (2008): 171.
- [9]
Hwang, Se-Min, Seok-Joon Yoon, Yoo-Mi Jung, Geun-Yong Kwon, Soo-Nam Jo, Eun-Jeong Jang, and Myoung-Ok Kwon, “Assessing the impact of meteorological factors on malaria patients in demilitarized zones in Republic of Korea,” Infectious Diseases of Poverty 5, no. 1 (2016): 20.
- [10]
- [11]
Jeong, Se Jin, Chang won Jang, Jin Hwan Jeon, Gi-Hun Kim, E-Hyun Shin, Young-Ran Ju, and Kyu-Sik Chang, “Insecticidal resistance and target gene mutation of Anopheles sinensis from four malaria risk areas in Republic of Korea,” In 2016 한국응용곤충학회 임시총회 및 추계학술발표회 [Korean Society of Applied Entomology] (2016): 131.
- [12]
Park, John J., Ah-Young Lim, Hyung-Soon Ahn, Andrew I. Kim, Soyoung Choi, David HW Oh, Owen Lee-Park et al, “Systematic review of evidence on public health in the Democratic People’s Republic of Korea.” BMJ Global Health 4, no. 2 (2019): e001133.
- [13]
- [14]
Lee, Won-Ja, Hyung-Hwan Kim, Soon-Mi Hwang, Mi-Young Park, Nam-Ryul Kim, Shin-Hyeong Cho, Tae-Sook In et al, “Detection of an antibody against Plasmodium vivax in residents of Gimpo-si, South Korea, using an indirect fluorescent antibody test,” Malaria Journal 10, no. 1 (2011): 19.
- [15]
USF Global Health Group’s Malaria Elimination Initiative, Eliminating Malaria in the Democratic People’s Republic Of Korea, Issue brief, Global Health Sciences, University of California, San Francisco (2015), accessed April 29, 2019, https://globalhealthsciences.ucsf.edu/sites/globalhealthsciences.ucsf.edu/files/pub/dprkorea2015-final.pdf.
- [16]
- [17]
World Health Organization, 134-36.
- [18]
Ibid., 112.